TF-Scan – non-invasive tear film assessment

Diagram 1: Schirmer’s test (Source, W. Sickenberger)

Diagram 2: BUT-Test
Dry eye
Dry Eye Syndrome is the result of inadequate wetting of the ocular surface. Dry eyes have numerous causes. Tear film production and composition play a prominent and important role. A disorder of the lipid layer leads to faster evaporation of the tear film and thus to dry eyes with the aforementioned complaints. Symptoms include stinging and scratching eyes, foreign body eye sensation, redness, increased sensitivity to light as well as contact lens and cosmetic intolerance. Working long hours at a monitor aggravates these problems in particular.
Tear film assessment
In terms of tear film assessment one can generally distinguish between invasive and non-invasive and between quantitative and qualitative methods. Methods are designated as invasive when they involve eye contact or application of fluorescein, for example. In contrast, noninvasive methods are contact-free.
Quantitative tear film analysis assesses the amount of tear film whereas qualitative tear film assessment provides information on tear film stability as well as tear film composition. The goal is to be able to determine the tear film quantity and quality non-invasively. Non-invasive measurements of the tear film do not irritate the eye, thus delivering more reliable results. Moreover, non-invasive methods are considerably more patient-friendly.
Schirmer's test (Diagram 1) is often used in practice to determine tear film quantity. This test involves hanging a strip of filter paper inside the lower lateral conjunctival sack. The litmus test strip becomes saturated with lacrimal fluid. The assessment is made after 5 minutes.
The invasive BUT test (Diagram 2), which entails applying fluorescein, is quite widely used for assessing tear film quality. The BUT test can be used to determine the break-up time of the tear film up to the point where dry patches occur. The longer the tear film needs to break up, the more stable it is. Both tests are invasive, however, and not always pleasant for the patient.
Qualitative assessment by using the OCULUS Keratograph
In close collaboration with JENVIS Research at the Jena University of Applied Sciences the TF-Scan (tear film scan) was developed for the OCULUS Keratograph (topographer). With this new software the tear film can be assessed qualitatively and quantitatively. Both measurements are taken non-invasively and thus in a more sanitary and patient-friendly way.

Diagram 3: Edge shift of placido rings (Source: D.Wiedemann, JENVIS Research Institute

Diagram 4: Automatic detection and evaluation |

Diagram 5: Color visualization of break-up time |
The break-up time of the tear film (quality) can be determined using the time-tested NIBUT procedure (non-invasive break-up time). Changes in the projected placido rings (edge shift of placido rings) indicates the break-up time of the tear film (Diagram 3 and 4). This evaluation is made automatically and the break-up time is represented in color. Dry patches which break up early on are marked in red. Color representation facilitates patient consultation considerably (Diagram 5).
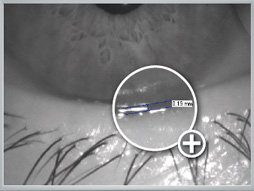
Diagram 6: Measured tear meniscus height
Quantitative assessment by using the OCULUS Keratograph
In addition the quantity of the tear film can be assessed non-invasively. To do this the tear meniscus height is determined. In comparison to Schirmer's test this method is much more pleasant for the patient. A tear meniscus height of 0.2 mm or less indicates that the amount of tear film is too small.
The tear meniscus height (quantity) can be measured and assessed quickly and easily after the data has been recorded using the keratograph software (Diagram 6).